Sick Woman Was Pregnant And Needed New Lungs But Docs Kept Her Alive Until Baby Could Be Born
Canadian doctors have managed to keep a pregnant woman in desperate need of a lung transplant alive using life-support equipment developed for COVID-19 patients so that she could give birth before having the operation.
Candice Cruise suffered from pulmonary hypertension with a high risk of death for the mother and baby which remained undiagnosed into the 21st week of pregnancy.
Under normal circumstances, medics would recommend termination of the pregnancy in order to save the mother’s life because of the extremely high risk.
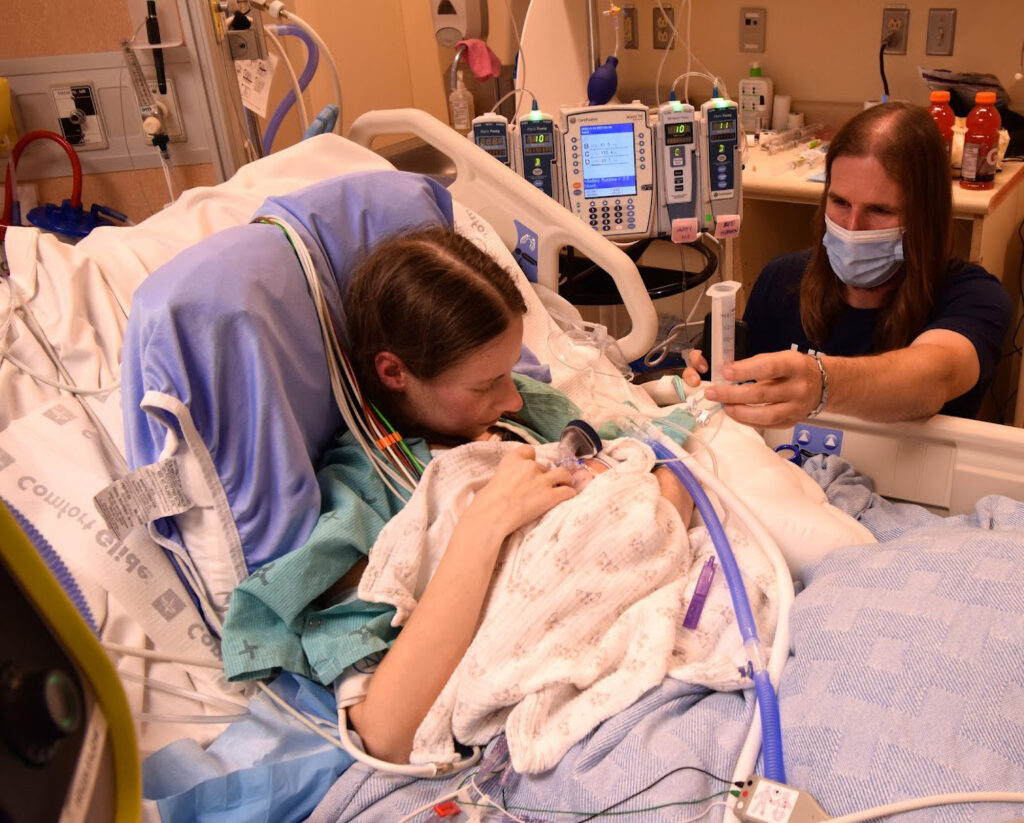
But a coordinated effort by teams including thoracic surgeons, respirologists, intensive care physicians, obstetricians, anaesthesiologists, cardiologists, and neonatologists together with acute care transport specialists at the Toronto General Hospital (TGH) came up with a pioneering strategy to connect the woman to an artificial lung device called a Novalung.
It artificially recreated the heart-lung blood flow allowing doctors to stabilise the pregnant woman until she got to the 29th week of pregnancy so that the baby could be delivered and she could then be transported for the urgent double-lung transplant.
The condition is a rare, life-threatening disorder, that leads to extremely elevated blood pressure of the arteries in the lungs.
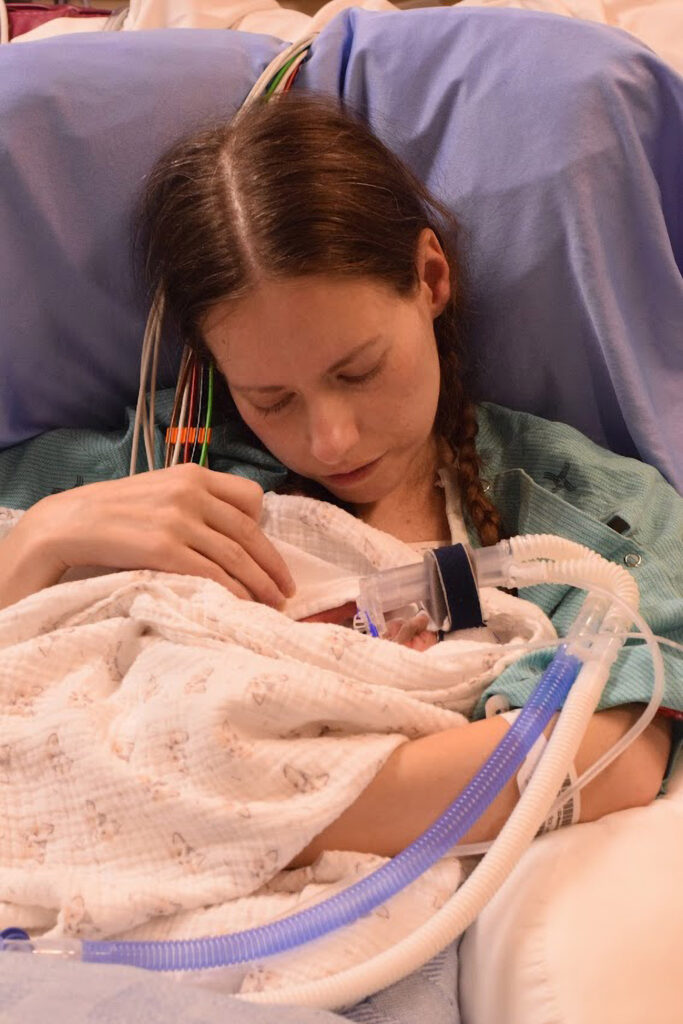
This increased pressure makes it difficult for the heart to pump blood through the lungs, which eventually causes the heart muscle to fail. The condition is especially dangerous during pregnancy since the growing baby naturally puts significant stress on the mother’s circulatory system.
Baby Cameron was born on 10th June 2021, and after he was stabilised, he was transferred to a regular ward before being allowed home.
His mother had the lung transplant carried out by the Toronto Lung Transplant Team at UHN’s Ajmera Transplant Centre, with the exact date kept secret in order to protect patient donor confidentiality.
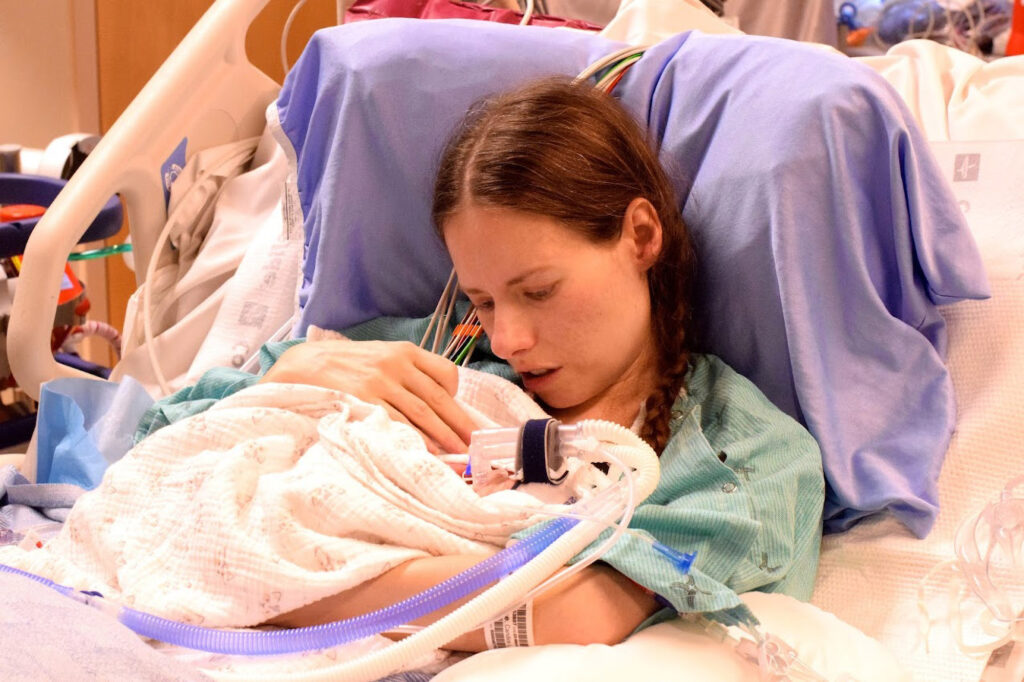
She was discharged home a month later. Cameron was discharged from St. Michael’s NICU in early September.
The family is now back at their home in the town of Midland, which is located in the central Canadian province of Ontario.
In a statement about the decision to fight for her child, Candice, whose age was not given, said: “I could feel the baby moving inside me, so strong. I knew there was nothing wrong with him, and I felt he had a good chance. I wasn’t ready to give up.”

Her husband Colin added: “We knew we had to prepare for the worst, which was very scary. As her husband, I wanted the safest approach to save Candice, but she kept fighting for our baby. So I put my trust in the doctors here, who are excellent. The whole team was amazing. They didn’t work only to keep Candice and Cameron alive, they really cared.”
Dr Shaf Keshavjee, UHN’s Surgeon in Chief and Director of the Toronto Lung Transplant Program at UHN’s Ajmera Transplant Centre, added: “This case really touched our team. It happened in part during the third wave of the pandemic when we were losing many young people to COVID. Seeing Candice and her baby have a positive outcome, against all odds, brought joy and a glimmer of hope to everyone involved in their care.
“We had never seen a case like this. Pulmonary Hypertension is a dangerous condition, even more so for pregnant women, with a high risk of death for both mother and fetus. We are incredibly happy that we were able to combine our expertise to be able to get Candice the support she needed to survive and have a healthy baby.”